What is Shock?
Shock is a life-threatening condition that occurs when there is an inability of the circulatory system of our body to supply oxygen to the cells.
Do you know about 1 in 5 people will die who suffer from shock?
When the body is unable to get blood flow to the organs, tissues, and cells, this becomes life-threatening, which leads to organ failure and ultimately death.
In the early stages, symptoms occur as the body attempts to compensate for blood loss.
What are the Signs and Symptoms of Shock?
In general, symptoms of shock may include:
- Chest pain
- Unconsciousness
- Nausea
- Low sugar levels
- Low blood pressure
- Pale, cool skin
- Dizziness
- Rapid pulse
- Dilated pupils
- Lightheadedness or fainting
- Weakness
- Agitation or anxiety
- Restlessness
- Blue-colored lips (gray if a person has a dark complexion)
- Blue-colored fingernails (gray in case of a dark complexion)
- Sweating
- Moist skin
Common Causes of Shock
Causes of shock may include:
- Sepsis
- Massive infection or an anaphylactic or severe allergic reaction may also cause shock from vasodilation.
- Accident causing heavy internal or external bleeding
- Severe infection in the body
- Physiological causes of shock are the heart failing to pump (heart attack or heart failure).
- Loss of blood volume or vessels dilating creates a vascular container capacity that is too great to be filled by available blood. This may be due to excessive bleeding or dehydration.
Want to learn different types of shock quickly? Check this Shock Explained in 120 Seconds with an Easy Video Animation
Different Types of Shock
The different types of shock are classified as:
- Compensated shock
- Decompensated shock
- Hypovolemic shock
- Cardiogenic shock
- Distributive shock
- Septic shock
- Anaphylactic shock
- Neurogenic shock
For your help, here is the detailed chart showing different types of shock. This chart shows differences in the pathogenesis and pathophysiology, which require group-specific, or, in other words, organ-specific treatment.
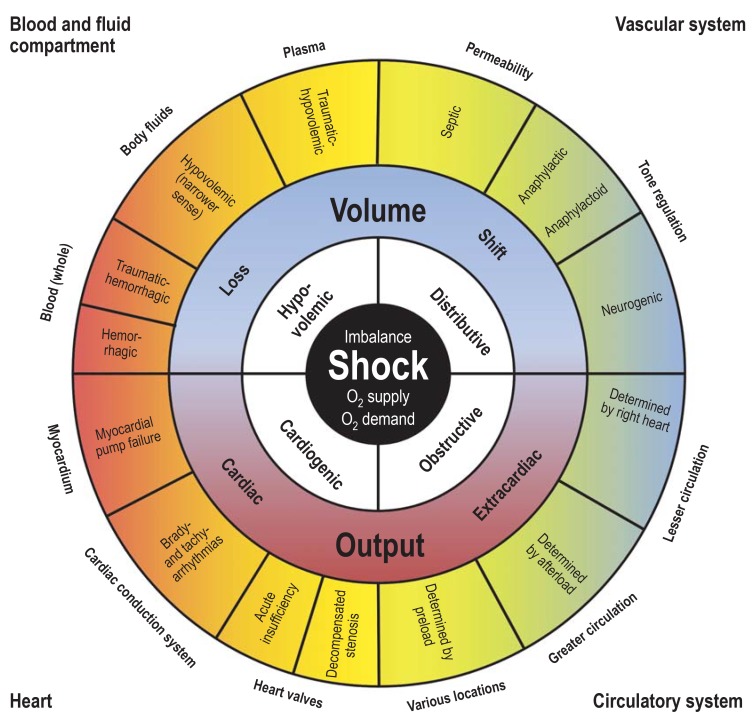
Image Credit: NCBI, The Nomenclature, Definition, and Distinction of Types of Shock
Now let’s look at all the different types of shock one by one below:
Compensated Shock
This type of shock includes an increased heart rate, increased respiration, and constriction of peripheral circulation. This results in pale cool skin. In infants and children, increased capillary refill time occurs.
Compensated shock signs and symptoms:
- Restlessness, agitation, and anxiety – the earliest signs of hypoxia
- Pallor and clammy skin – this is because of microcirculation
- Nausea and vomiting – this occurs because of decreased blood flow to the GI system
- Thirst
- Delayed capillary refill
- Narrowing pulse pressure
Decompensated Shock
This type of shock starts with low blood volume or a lack of perfusion. Shock is irreversible when perfusion to the organs cannot be restored.
Cell damage occurs, especially in the liver and kidneys. Even if vital signs are restored, irreparably damaged organs may cause death.
Decompensated shock signs and symptoms:
- Alterations in mental status
- Tachycardia – a heart rate over 100 beats per minute
- Tachypnea – abnormally rapid breathing
- Labored and irregular breathing
- Weak to absent peripheral pulses
- A decrease in body temperature
- Cyanosis – a bluish-purple hue to the skin
Hypovolemic shock
Hypovolemic shock occurs when the patient loses about one-fifth (1/5) or more of the normal amount of blood from the body. Hypovolemic shock is also known as hemorrhagic shock.
Hypovolemic shock signs and symptoms:
- Agitation or anxiety
- Cool and clammy skin
- Confusion
- Decreased or no urine output
- Generalized weakness
- Pallor (pale skin color)
- Rapid breathing
- Sweating, moist skin
- Lack of responsiveness or unconsciousness
Hypovolemic shock treatment
Manage the source of bleeding as quickly as possible and fluid replacement.
In controlled hemorrhagic shock (CHS) where the source of bleeding has been occluded fluid substitute is aimed toward the normalization of hemodynamic parameters.
In uncontrolled hemorrhagic shock (UCHS) wherein bleeding has briefly stopped – due to hypotension, vasoconstriction, and clot formation – the fluid therapy is aimed toward restoration of the radial pulse, restoration of the sensorium, or acquiring a BP of 80 mmHg by aliquots of 250 ml of lactated Ringer’s solution (hypotensive resuscitation).
When evacuation time is shorter than one hour (often city trauma) instant evacuation to a surgical facility is indicated after airway and breathing. (Source)
Cardiogenic Shock
Cardiogenic shock occurs during a myocardial infarction or heart attack; damaged heart muscle; or electrical malfunctioning decreases the strength of the heart’s contractions causing a slow-fast or irregular heartbeat.
Cardiogenic shock signs and symptoms:
- Lack of consciousness
- Fast respiration
- Extreme shortness of breath
- Sudden, fast heartbeat (tachycardia)
- Weak pulse
- Low blood pressure (systemic hypotension)
- Sweating
- Pale skin
- Cold hands or feet
- Urinating lower than regular or by no means
In cardiogenic shock blood pressure is decreased with a systolic blood pressure of less than 90 mmHg or a decrease in mean blood pressure by 30 mmHg.
Causes of cardiogenic shock
Cardiogenic shock is caused by an absence of oxygen in your heart. This often occurs due to a heart attack, which damages its major pumping chamber (left ventricle). Without oxygenated blood flowing to that area of your heart, the heart muscle can weaken and go into cardiogenic shock.
Not often, does injury to your heart’s right ventricle, which sends blood to your lungs to get oxygen, result in cardiogenic shock.
Different possible causes of cardiogenic shock include:
- Myocarditis
- Endocarditis
- Weakened heart from any trigger
- Drug overdoses or poisoning with substances that may have an effect on your heart’s pumping capability
Manifestations of cardiogenic shock
Manifestations of cardiogenic shock include quick restoration of blood pressure and heart function while taking patients in an ambulance or in an emergency room.
Emergency medical treatment may include enriched oxygen in a tube or masks; respiratory assistance (ventilator); intravenous (IV) fluids and medicines to boost blood pressure or heart function.
There may be an array of medicines that may be given to deal with cardiogenic shock. These differ relying upon the reason for it and will include:
- Thrombolytic medicine to dissolve coronary artery clots (“clot-busting” drugs similar to tPA)
- Anti-clotting agents to stop new clots (e.g., aspirin, clopidogrel, heparin)
- Medication to extend the heart’s pumping capacity (e.g., dobutamine, dopamine, epinephrine)
- Different potential therapies include oxygen to guard heart tissue; nitroglycerin to widen coronary vessels; medication to lower the heart’s workload and pain, relieve anxiety, or regulate heart rhythm
Distributive Shock
Distributive shock occurs when there is an abnormal distribution of blood to tissues and organs. Distributive shock has further three types; septic, anaphylactic, and neurogenic shock.
Distributive shock signs and symptoms:
- Tachypnea
- Tachycardia
- Low to normal blood pressure
- Decreased urine output
- Decreased level of consciousness
Septic Shock
Septic shock is the most common cause of distributive shock and is caused by an overwhelming systemic infection that is resistant to the immune system, and results in vasodilation and hypotension.
There are three stages of sepsis:
Stage 1:
In this stage, the infection reaches the bloodstream and results in inflammation in the body.
Stage 2:
At this stage, sepsis becomes severe. At this point, the infection is severe and starts affecting the functions of your body organs, such as the heart, brain, and kidneys.
Stage 3:
Stage 3 of sepsis is considered the most dangerous stage. In this, the patient experiences a significant drop in blood pressure that can lead to organ failures, such as heart or respiratory failure, stroke, failure of other organs, and death
Treatment of Septic Shock
For adults, the patient is admitted to an intensive care unit (ICU). In ICU, treatment of infection is started and on the other hand body functions and organs are supported. In some cases, treatment may be started in the emergency department or ER.
Treatment of sepsis may include:
- Oxygen therapy
- Intravenous fluids are given
- Medication to increase blood pressure (vasopressor medications)
- Intravenous antibiotics to cure the infection
- Surgery (in some cases)
- Corticosteroids
Anaphylactic Shock (Anaphylactoid shock)
A severe reaction to an allergen causes anaphylactic shock. This severe reaction leads to the release of histamine that causes extensive vasodilation and hypotension.
Anaphylactic shock symptoms:
- Lightheadedness or faintness
- Difficulty breathing – such as fast, shallow breathing
- Wheezing
- Rapid heartbeat
- Clammy skin
- Confusion and anxiety
- Loss of consciousness or collapse
- Itchy, raised rash (hives)
- Feeling or being sick
- Swelling (angioedema)
- Stomach pain
Treatment of Anaphylactic Shock
Anaphylaxis is a medical emergency, this requires immediate medical treatment. If someone has the symptoms of anaphylaxis, you should do the following:
- Use adrenaline auto-injector – use it only if you know how to use it properly
- Call emergency helpline 911 or 999 for an ambulance immediately – you should call even if they start to feel better
- Identify the trigger, if possible, and remove it – e.g., carefully remove anything stuck in the skin that has caused the reaction.
- Lie the patient down flat – unless they are unconscious, pregnant, or having breathing difficulties
- Give another injection after 5-15 minutes if another auto-injector is available and the symptoms persist
If you are having an anaphylactic reaction, you can follow these steps yourself if you feel you can do it easily.
Treatment of anaphylactic shock in the hospital includes:
- You will be admitted for 6-12 hours, because symptoms may occur again sometimes.
- In case of breathing difficulty, an oxygen mask may be used.
- Intravenous fluids may be given to help increase blood pressure
- Antihistamines and steroids may be used to help relieve symptoms
- Blood investigations may be carried out to confirm anaphylaxis
Neurogenic Shock
The neurogenic shock may result from the uncontrolled dilation of vessels due to nerve paralysis in spinal cord injuries. There is no blood loss, but the vessel dilation increases the capacity of the circulatory system and available blood can no longer fill it.
Neurogenic shock symptoms:
In this type of shock, low blood pressure is one of the core symptoms of neurogenic shock. However, this condition may cause several other symptoms.
In normal cases, the symptoms of neurogenic shock include:
- Dizziness
- Nausea
- Vomiting
- Blank stares
- Fainting
- Increased sweating
- Anxiety
- Pale skin
In very severe cases, neurogenic shock symptoms may include:
- Breathing difficulty
- Pain in chest
- Weakness from irregular blood circulation
- Slow heart rate or bradycardia
- Faint or weak pulse
- Cyanosis, or discoloration of lips and fingers
- Hypothermia, or decrease in body temperature
If neurogenic shock is left untreated, it can cause irreversible tissue damage and death. Seek immediate medical treatment, if you begin experiencing any of these symptoms mentioned above.
ALSO READ: How to Improve Heart Health by Avoiding These 5 Habits
Management of Shock
Overall management explains in general how you can treat different types of shock. Before proceeding with the shock treatment, your first and foremost course of action should be to call 911 or any other local emergency number in your respective country to get immediate medication attention.
You need to stay with the person. You should also stay on the call with the emergency team as they may provide you with important instructions to handle the situation at the time.
For almost all different types of shock, the first line of treatment is fluid resuscitation. This means you should provide the patient with a large volume of IV fluids. As a result of this, the BP of the patient will increase.
IV fluids may be administered by the ambulance staff when they are on their way to the hospital or may be administered in the emergency room.
Do not administer fluids by mouth. There is a chance of choking in case the patient gets unconscious. Do not do this even if the patient complains of thirst or dry mouth.
After you have called 911 or your local emergency, you can perform the following first aid:
- Lay the patient down straight
- Slightly raise the legs & feet and make sure the patient doesn’t feel pain
- Keeping the patient still is preferred; don’t move unless it is very necessary.
- If you see there are no signs of life like breathing, movement or coughing, etc. then start Cardiopulmonary Resuscitation (CPR), if you have training.
- The patient may be wearing tight clothes, lose them immediately to prevent the patient from suffocation.
- It may be due to an external injury, you should apply direct pressure to the wound site to prevent blood loss.
- If the patient feels chills or is very cold, cover with a blanket.
- The patient may show signs of bleeding from the mouth or vomiting, which may cause choking. To prevent this, turn the patient aside. Make sure this doesn’t cause spinal injury in case the patient is injured from the back.
In Summary
Shock or hypoperfusion is a life-threatening medical condition in which there is reduced oxygen supply to the cells through the circulatory system. This causes a reduced blood supply to the organs, as a result, they stop functioning. There are different types of shock, compensated, decompensated, hypovolemic or hemorrhagic, cardiogenic, distributive, septic, anaphylactic, and neurogenic. Medical treatment depends on the different types of shock a person encounters. As an Emergency Medical Technician (EMT), you do not need to diagnose the type; instead, you must recognize and treat it whenever there is a mechanism of injury or signs that indicate the possibility of shock. Always call the emergency helpline in your local area of your respective country.
ALSO READ:
The 7 Best Ayurvedic Herbs with Amazing Health Benefits
Nutrition Facts About Oatmeal | Complete Guide & Health Benefits
The 6 Best Hearing Loss Treatment Options To Help You Fight Back


